Medically reviewed by Dr. Samuel Davidoff, MD, Board-Certified Gastroenterologist & Hepatologist | 18+ Years Experience | Last Updated: April 2026
Quick Answer
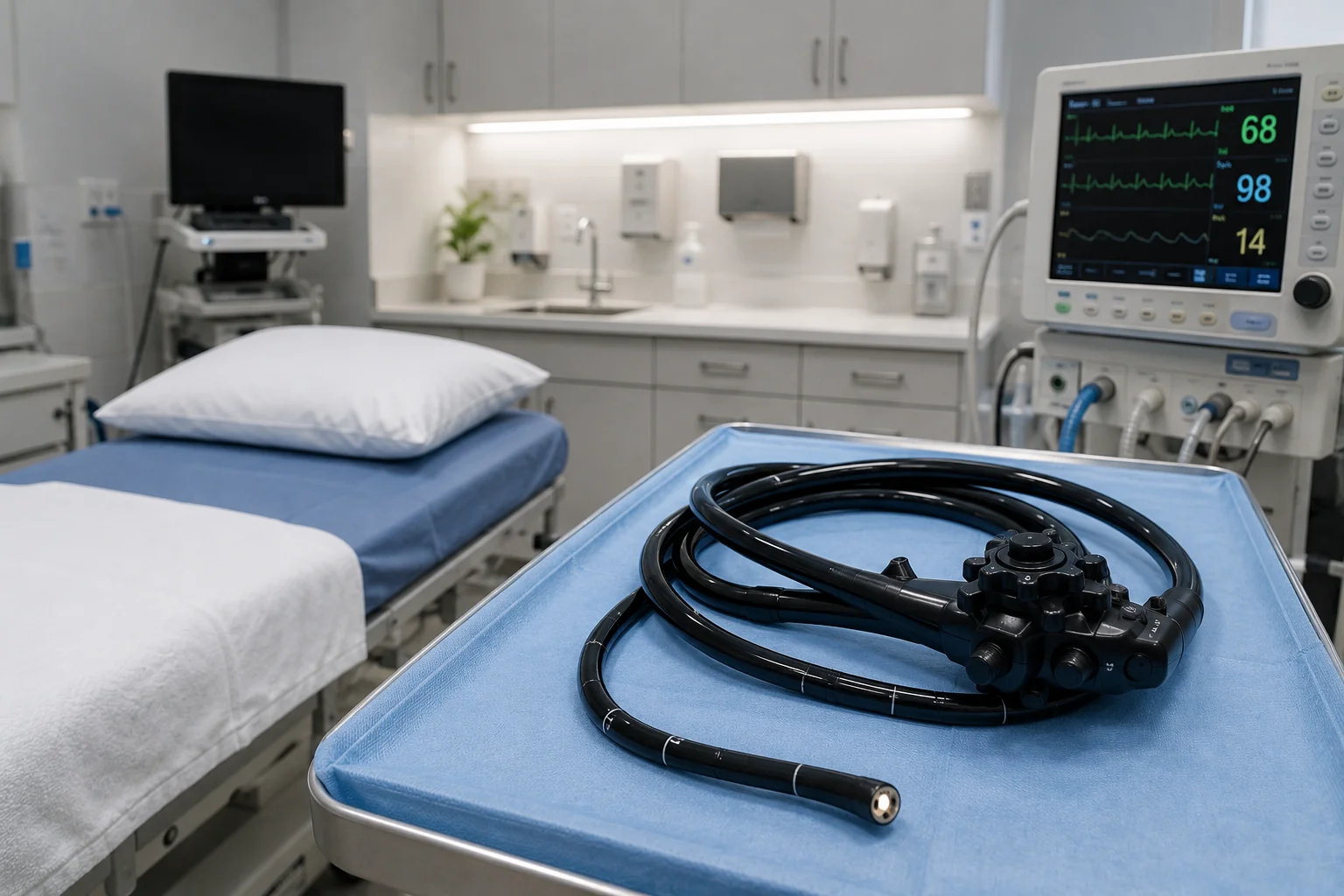
No, an upper endoscopy is not painful. The procedure is performed under deep sedation with propofol, so you are completely asleep and feel nothing during the 5 to 7 minutes of actual endoscope time. You will not gag, will not feel the tube, and will not have any memory of the procedure itself. Total time at the office is about 1 to 1.5 hours including IV placement, the procedure, and the 20 to 30 minute recovery from sedation. At Gastroenterology and Nutrition P.C. in Forest Hills, all upper endoscopies are performed at our AAAASF-certified facility under propofol sedation administered by a dedicated anesthesiologist.
Most patients walk into a first endoscopy consultation with the same question: is this going to hurt? The honest answer, the one our patients hear from Dr. Yuriy Israel before every procedure, is that it does not. The pain question comes up because endoscopy involves a flexible tube being passed through the mouth, down the esophagus, and into the stomach and the first part of the small intestine. That sounds uncomfortable in the abstract. In practice, with modern propofol sedation, the patient is fully asleep before any of that happens and wakes up when it is over.
This guide explains exactly what propofol does, what you will and will not feel, what to expect during the procedure, the small things people often worry about (gagging, coughing, breathing), and what recovery actually looks like.
The Direct Answer From Our Endoscopist
Per Dr. Yuriy Israel, MD, board-certified gastroenterologist at Gastroenterology and Nutrition P.C.:
“No, it is not. You’re asleep during the whole procedure, so you do not feel any pain or discomfort.”
Dr. Yuriy Israel, MD, Board-Certified Gastroenterologist, Forest Hills
That is the headline. The rest of this guide is the detail behind it.
Why Propofol Changes the Experience
Propofol is a short-acting intravenous anesthetic that produces deep, predictable sedation in seconds and wears off in 15 to 20 minutes after the medication is stopped. It is the standard of care for endoscopic procedures at most modern GI practices, and it is what allows endoscopy to be a procedure that patients describe as “I don’t remember anything” rather than a procedure they dread.
Per Dr. Israel: “99% of the time, you won’t gag because we use an anesthetic called propofol, which puts you in a deep sleep and suppresses the gag reflex. In places where they use conscious sedation instead of propofol, you may gag, but when we use propofol, you will not.”
This is the key distinction. Some older or lower-cost practices still use “conscious sedation” with medications like midazolam and fentanyl, which leave the patient in a lighter state where the gag reflex can fire. Propofol-based deep sedation, administered by a dedicated anesthesiologist, suppresses the gag reflex entirely. Patients sleep through the procedure with no awareness, no discomfort, and no memory.
What Actually Happens, Minute by Minute
From the moment you arrive at our Forest Hills office to the moment you leave, the typical timeline:
- Minutes 0-15: Check-in. Paperwork, verify ID and insurance, confirm fasting status (no food or drink for 8 to 10 hours before the procedure).
- Minutes 15-20: Pre-procedure prep. Change into a gown if requested (more on this below), the anesthesiologist places an IV in your hand or arm.
- Minutes 20-25: Sedation. The anesthesiologist injects propofol through the IV. Patients describe falling asleep within seconds, similar to general anesthesia for a minor surgery.
- Minutes 25-32: The procedure. The actual endoscopy takes 5 to 7 minutes. You are fully asleep. The endoscopist passes the flexible scope through the mouth and inspects the esophagus, stomach, and the first part of the small intestine (duodenum). Biopsies are taken if anything looks abnormal.
- Minutes 32-60: Recovery. The propofol wears off. You wake up, feel a little groggy for the first few minutes, and then return to baseline. Total recovery time is typically 20 to 30 minutes.
- Minutes 60+: Discharge. The doctor reviews the visual findings with you immediately. You receive a copy of the report. You can walk out and go home (with a designated driver) within an hour and a half of arrival.
Per Dr. Israel: “Immediately after the procedure, you may feel a little groggy, but once the anesthesia wears off after 15-20 minutes, you will feel like your normal self.”
“But What About…”: The Common Worries
Most pre-endoscopy anxiety comes down to a few specific worries. Here are the direct answers:
Will I gag when the tube goes down?
No. Per Dr. Israel: “99% of the time, you won’t gag because we use an anesthetic called propofol, which puts you in a deep sleep and suppresses the gag reflex.” The 1% case is when a patient has unusually rapid metabolism of propofol, in which case the anesthesiologist adjusts the dose. You will not be aware of any gagging if it happens because the sedation is too deep for awareness.
Will I be able to breathe?
Yes, normally. Per Dr. Israel: “We put a Bite Block in your mouth, which keeps your mouth open and protects your teeth. You can breathe through your nose or mouth, whichever is comfortable.” The Bite Block is a small soft plastic guard that sits between your teeth. The endoscope passes through it. Your airway is unobstructed and your breathing is monitored continuously by the anesthesiologist.
What if I cough during the procedure?
Per Dr. Israel: “You may cough during an upper endoscopy because, on rare occasions, some saliva may get into your throat and tickle your vocal cords. This may cause coughing.” This is rare and managed by the anesthesiologist in the moment. You will not be aware it is happening.
Do I have to undress?
Per Dr. Israel: “Yes, you are fully clothed. We do not ask you to disrobe or take off any clothing. You come in your street clothes, we perform the procedure, and then you go home.” Some patients are asked to wear a gown for comfort during recovery, but you do not need to undress for an upper endoscopy.
Will I be embarrassed by anything I might say or do under sedation?
Propofol is not the same as the “talking under anesthesia” effect people remember from older sedatives or wisdom-tooth videos. Patients are deeply asleep and do not talk, sing, or remember anything during the procedure itself. Recovery is brief and matter-of-fact.
Will my throat hurt afterward?
A mild sore throat for the rest of the day is possible but uncommon. Most patients have no throat irritation at all. If it does occur, it resolves within 24 hours and does not need treatment.
Is it normal to vomit afterward?
Per Dr. Israel: “No, it is not normal to vomit. It’s a very benign procedure, and you should not have any gag reflex once you wake up.” If you do feel nauseous, mention it to the recovery team. It is not a routine reaction to the procedure itself.
When Endoscopy Is Recommended
Per Dr. Israel: “An upper endoscopy can be performed for a number of reasons. Primarily, if you’re having abdominal pain, especially in the epigastric area, which is right below your rib cage, we can see if you have an ulcer, gastritis, or any inflammation. If you have chronic heartburn, which can lead to changes in the lining of your esophagus, an upper endoscopy allows us to see what’s going on there.”
The standard list of indications for upper endoscopy:
- Heartburn that does not respond to over-the-counter or prescription antacids
- Long-standing reflux to evaluate for Barrett’s esophagus
- Persistent upper abdominal pain, especially worse after meals (rule out ulcer)
- Difficulty swallowing or feeling like food is “stuck” in the chest
- Vomiting blood
- Pitch-black stools (sign of upper GI bleeding)
- Suspected celiac disease, H. pylori infection, gastritis
- Follow-up of previously identified abnormalities
Per Dr. Israel on what endoscopy can detect: “It can detect anything from Barrett’s esophagus, esophageal rings, various infections of the esophagus, gastritis, stomach ulcers, stomach cancer, stomach polyps, and duodenal issues. It can also detect celiac disease, Crohn’s disease, and other inflammatory or autoimmune processes that affect the stomach or small intestine.”
Pre-Procedure Preparation (8 to 10 Hours of Fasting)
Per Dr. Israel: “The preparation is very simple. You cannot eat or drink anything for at least 8 to 10 hours before the procedure.”
The full prep checklist:
- The day before: Eat and drink normally until 10 PM (or per your specific instructions). After 10 PM, no more food or drink.
- Morning of the procedure: No eating, no drinking. This includes water, coffee, gum, mints, and lozenges. Per Dr. Israel: “No, you cannot drink anything for at least 8 to 10 hours before the procedure.”
- Brushing your teeth: Per Dr. Israel: “Absolutely. We encourage good oral hygiene before the procedure.” Do not swallow water while brushing.
- GLP-1 medications (Ozempic, Mounjaro, Wegovy): Stop at least 1 week before the procedure per Dr. Israel and current ASA guidance. These medications slow gastric emptying and can leave food in the stomach despite fasting.
- Other medications: Most regular medications can be taken with a small sip of water the morning of the procedure. Confirm with our office.
- Arrival: Come 15 minutes before your scheduled time for paperwork.
- Designated driver: You cannot drive after sedation. Arrange transportation in advance.
After the Procedure: What You Can and Cannot Do
Per Dr. Israel: “As soon as you wake up and feel up to it, you can eat whatever you want. The only recommendation is to avoid alcohol for 24 hours after the procedure.”
The recovery rules:
- Eating: Resume normal diet as soon as you feel hungry.
- Drinking: Yes, but no alcohol for 24 hours.
- Driving: No driving for 24 hours after sedation. Have someone pick you up.
- Work: Most patients return to work the next day. Some take the rest of the procedure day off.
- Heavy lifting and exercise: Resume normal activity the next day unless biopsies were taken in unusual locations.
- Medications: Resume per your physician’s instructions.
When to Call Our Office After Endoscopy
True complications from upper endoscopy under propofol sedation are rare (less than 1 in 1,000), but call us if you experience any of the following in the 24 to 48 hours after your procedure:
- Severe abdominal pain (mild discomfort or bloating from air introduced during the procedure is normal and resolves within hours)
- Persistent vomiting
- Vomiting blood or coffee-ground-like material
- Black, tarry stools
- Fever above 100.4°F
- Difficulty breathing or swallowing that gets worse
- Chest pain
For routine post-procedure questions, call our office at (718) 261-0900.
Why Forest Hills Patients Choose Our Practice
Gastroenterology and Nutrition P.C. is an AAAASF-certified facility at 108-16 72nd Avenue, 2nd Floor, Forest Hills, Queens NY 11375. AAAASF certification (American Association for Accreditation of Ambulatory Surgery Facilities) is the highest standard for outpatient surgical facilities and verifies that our equipment, staff training, sedation protocols, and emergency preparedness meet rigorous national benchmarks.
Our patients come from Forest Hills, Rego Park, Kew Gardens, Elmhurst, Jackson Heights, and across Queens. We perform upper endoscopies and colonoscopies on-site, including Sunday hours for patients who cannot take time off during the week. Our team speaks English, Russian, and Spanish (Dr. Israel) and Russian (Dr. Davidoff and our nurse practitioner Emanuel Yaakobov).
Schedule an Endoscopy Consultation
Or call (718) 261-0900
Frequently Asked Questions
How long does an upper endoscopy take?
Per Dr. Israel: “The procedure itself takes anywhere between five to seven minutes. However, the entire process may take about an hour to an hour and a half, including putting in the IV, performing the procedure, and the recovery period after anesthesia.”
Will I feel anything during the procedure?
No. The propofol used for sedation produces deep, predictable sleep. Patients have no awareness of the endoscope passing through the mouth, esophagus, or stomach, and no memory of the procedure itself.
Is propofol safe?
Yes, when administered by a trained anesthesiologist in a properly equipped facility. Propofol is the standard sedation agent used in endoscopy at AAAASF-certified facilities like Gastroenterology and Nutrition P.C. It produces faster, more predictable, and more comfortable sedation than older “conscious sedation” protocols.
Can I drive home after my endoscopy?
No. Sedation effects can persist for hours even after you feel “back to normal.” Plan for a designated driver to take you home and avoid driving, operating machinery, or making important legal or financial decisions for the rest of the day.
What is the difference between deep sedation and general anesthesia?
Deep sedation with propofol keeps you in a state where you are unaware of the procedure but breathing on your own. General anesthesia involves a breathing tube and is used for major surgery. Endoscopy uses deep sedation, not general anesthesia, which is why recovery is faster and the experience is much lighter.
How soon can I eat after an upper endoscopy?
Per Dr. Israel: “As soon as you wake up and feel up to it, you can eat whatever you want. The only recommendation is to avoid alcohol for 24 hours after the procedure.”
This information is provided for educational purposes and is not a substitute for professional medical advice, diagnosis, or treatment. Please schedule a consultation with our team to discuss your individual needs.