Ulcerative Colitis
Ulcerative colitis is a chronic inflammation of the rectum and colon. It is part of a group of diseases known as inflammatory bowel disease. Ulcerative colitis causes inflammation and ulcers in the lining of the rectum and colon. The ulcers can flare up and cause painful symptoms which can eventually lead to colon cancer.
Medically reviewed by Dr. Samuel Davidoff, MD, Board-Certified Gastroenterologist & Hepatologist | 18+ Years Experience | Last Updated: April 2026
Your Ulcerative Colitis Specialists in Forest Hills, Queens
Dr. Samuel Davidoff, MD, has managed patients with ulcerative colitis for over 18 years. Board-certified in both Gastroenterology and Hepatology, Dr. Davidoff founded Gastroenterology and Nutrition, P.C. with a treatment philosophy grounded in finding root causes and working with each patient to build a clear, manageable plan. His approach to UC focuses on achieving remission through personalized medication selection and close monitoring.
Dr. Yuriy Israel, MD, board-certified in Gastroenterology and Internal Medicine, brings over 15 years of experience in digestive disease management. Together, they provide ongoing IBD care from diagnosis through long-term maintenance.
Our Forest Hills office is equipped for in-office colonoscopy in an AAAASF-accredited procedure suite, which means diagnostic evaluations and surveillance colonoscopies happen in a setting that meets hospital-level safety standards. We also offer capsule endoscopy for patients who need imaging beyond what traditional colonoscopy can reach. Nurse practitioner Emanuel Yaakobov, FNP-BC, supports patient care and follow-up throughout the treatment process.
Causes of Ulcerative Colitis
While ulcerative colitis usually begins between the ages of 15 and 30, many people over the age of 50 can also develop the disease. Thought to be an autoimmune disease, the cause of ulcerative colitis is unknown, yet there is a tendency for patients with ulcerative colitis to have a close family relative with the same disease. Stress and other environmental factors may aggravate symptoms of ulcerative colitis, they are not the cause of the disease.
Patient Safety
Ulcerative colitis is a chronic condition that benefits from specialized gastroenterology care. At Gastroenterology & Nutrition P.C. in Forest Hills, Queens, our board-certified gastroenterologists, Dr. Samuel Davidoff and Dr. Yuriy Israel, provide expert UC diagnosis and ongoing management with decades of combined clinical experience. Timely diagnosis and the right treatment strategy can help you achieve and maintain remission.
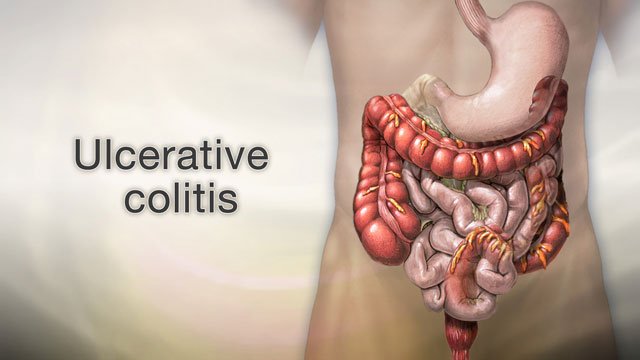
Symptoms of Ulcerative Colitis
Symptoms of ulcerative colitis occur in flare-ups that can be sudden and severe or begin gradually with mild symptoms. Depending on the severity of the inflammation, people may experience the disease differently. Common symptoms of ulcerative colitis may include the following:
- Abdominal pain
- Bloody diarrhea
- Fever
- Fatigue
- Weight loss
- Loss of appetite
- Joint pains
- Anemia
- Rectal pain
- Rectal bleeding
Diagnosis of Ulcerative Colitis
After conducting a thorough medical evaluation, various tests will be performed to confirm diagnosis. These tests may include:
- Blood test
- Stool test
- Colonoscopy with biopsy
- CT Scan
- Barium enema
- Flexible sigmoidoscopy
- X-ray


Treatment of Ulcerative Colitis
Treatment for ulcerative colitis depends on the severity of the disease, but may include the following treatment methods:
- Drug therapy to induce and maintain remission
- Hospitalization to treat severe symptoms
- Surgery to remove the colon and rectum
- Adjustments to diet
Stress management
Many people with severe ulcerative colitis may have their colons removed due to excessive bleeding and a high risk of developing colon cancer.
People with ulcerative colitis may experience periods of remission that last months or even years. The doctor can help determine which treatment option will work well based on the condition.
Living with Ulcerative Colitis
Ulcerative colitis symptoms overlap with many other conditions, so getting an accurate diagnosis early makes a real difference in outcomes. Contact a gastroenterologist if you experience:
- Bloody diarrhea lasting more than a few days
- Persistent abdominal pain with changes in bowel habits
- Frequent, urgent bowel movements that interfere with daily life
- Unexplained weight loss or fatigue
- Rectal bleeding of any kind
If you’ve already been diagnosed with UC, call our office if you notice new symptoms, increasing frequency of flares, or if your current medications seem less effective. Early adjustments often prevent full-blown flares. Reach us at (718) 261-0900.
Common Questions About Ulcerative Colitis
Q: What are the early signs of ulcerative colitis?
A: The earliest sign is usually bloody diarrhea or blood mixed with stool. Many people also notice increased urgency, needing to reach a bathroom quickly and frequently. Mild abdominal cramping on the left side is common early on. Some patients initially dismiss these symptoms as a stomach bug. If bloody diarrhea lasts more than a week, it’s time to see a gastroenterologist for evaluation.
Q: Can ulcerative colitis be cured?
A: There’s currently no medical cure for ulcerative colitis, but effective treatments can put the disease into long-term remission where you have no symptoms. Many patients live normal, active lives on maintenance medication. The only definitive cure is surgical removal of the colon (colectomy), which eliminates the disease entirely because UC only affects the large intestine. Most patients manage well with medication alone.
Q: What foods should I avoid with ulcerative colitis?
A: During a flare, many patients benefit from avoiding high-fiber foods, raw vegetables, seeds, nuts, spicy foods, caffeine, and alcohol. Dairy causes problems for some UC patients but not all. During remission, most people can eat a broader diet. There’s no one-size-fits-all UC diet. Keeping a food diary helps identify your personal triggers, and our team can help you develop a nutrition plan that works.
Q: How is ulcerative colitis different from Crohn's disease?
A: Both are inflammatory bowel diseases, but they affect different areas. UC only involves the large intestine and rectum, and inflammation is continuous along the colon lining. Crohn’s can appear anywhere from the mouth to the anus, often affects the small intestine, and causes patchy inflammation that goes deeper into the bowel wall. Treatment strategies overlap but differ in important ways. Accurate diagnosis determines the right approach.
Q: How often do I need a colonoscopy with ulcerative colitis?
A: Surveillance colonoscopy frequency depends on your disease extent and duration. Generally, patients with UC beyond the rectum should begin surveillance colonoscopies 8 years after diagnosis, then every 1-3 years depending on risk factors. Patients with pancolitis or those with a family history of colorectal cancer may need more frequent screening. Dr. Davidoff sets an individualized surveillance schedule based on your specific situation.
Disclaimer: This information is provided for educational purposes and is not a substitute for professional medical advice, diagnosis, or treatment. Please schedule a consultation with our team to discuss your individual needs.
