Hemorrhoids
Hemorrhoids are swollen veins in the anal canal. In their normal state, these veins provide cushioning during bowel movements. They can, however, swell after lifting, straining, constipation, passing of hard stools or diarrhea, or pregnancy. Hemorrhoids are not life-threatening, but they can be painful. If swelling persists, the veins may become permanently stretched (prolapsed).
Medically reviewed by Dr. Yuriy Israel, MD, Board-Certified Gastroenterologist | 15+ Years Experience | Last Updated: April 2026
Your Hemorrhoid Specialists in Forest Hills, Queens
Dr. Yuriy Israel, MD, and Dr. Samuel Davidoff, MD, have treated thousands of patients with hemorrhoids across more than 15 combined years at Gastroenterology and Nutrition, P.C. Both are board-certified gastroenterologists who specialize in minimally invasive hemorrhoid treatment.
Dr. Israel brings board certification in both Gastroenterology and Internal Medicine, with a focus on evidence-based treatment that gets patients back to normal life quickly. Dr. Davidoff, a board-certified Gastroenterologist and Hepatologist, founded the practice with a philosophy of finding root causes and choosing the least invasive approach first.
Our Forest Hills office includes an AAAASF-accredited procedure suite where we perform rubber band ligation, infrared coagulation, and diagnostic evaluations on-site. AAAASF accreditation means our facility meets the same safety and equipment standards as hospital-based surgical centers. That translates to fewer complications and a safer experience for patients who need in-office procedures. You won’t need a hospital visit for most hemorrhoid treatments.
Types of Hemorrhoids
There are two kinds of hemorrhoids: internal and external. The dentate line along the circular anus muscle divides the interior nerve canal, which has no nerve endings, from the anal opening and exterior areas, which do have nerve endings.
01. Internal Hemorrhoids
✔ Located inside the anal canal, above the dentate line.
✔ Usually painless because the area has no nerve endings.
✔ Can cause bleeding, and if they swell or protrude, may lead to pain and discomfort.
02. External Hemorrhoids
✔ Found outside the anal opening, below the dentate line.
✔
Painful and itchy, as the area has many nerve endings.
✔
May cause swelling, irritation, and sometimes bleeding.
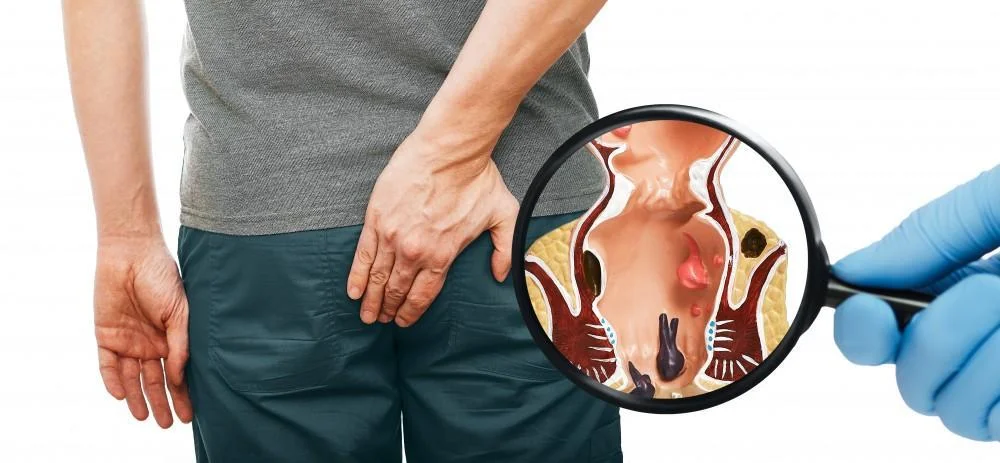
Symptoms of Hemorrhoids
Hemorrhoid symptoms vary based on factors like age, anatomy, heredity, and duration of the condition. Common symptoms include bleeding, itching, burning, pain during bowel movements, and a feeling of fullness or a lump around the anus.
At Gastroenterology & Nutrition P.C. in Forest Hills, Queens, our board-certified gastroenterologists, Dr. Yuriy Israel and Dr. Samuel Davidoff, offer in-office hemorrhoid treatment including rubber band ligation. Common symptoms include:
- Bleeding
- Itching
- Burning sensation
- Discomfort during bowel movements
- Feeling of fullness or presence of a mass in or on the anus
Causes and Risk Factors
Hemorrhoids develop when pressure increases on the blood vessels in the rectal and anal area. Common causes include:
- Straining during bowel movements, especially with chronic constipation
- Sitting on the toilet for extended periods
- Chronic diarrhea
- Pregnancy and childbirth (increased abdominal pressure)
- Obesity
- Low-fiber diet
- Heavy lifting on a regular basis
- Aging, which weakens the supportive tissue around rectal veins
A sedentary lifestyle and not drinking enough water also contribute. Some patients have a genetic predisposition to weaker vein walls, which makes hemorrhoids more likely.
Treatment for Hemorrhoids
Hemorrhoids should be treated only if they are painful or cause complications. To choose an appropriate treatment, the cause or causes need to be determined. Making changes to diet and fluid intake, toilet habits and exercise can relieve symptoms and prevent recurrence. Relief can also be found by treating related problems, such as diarrhea and constipation, that irritate the hemorrhoid(s) and affected areas.
Beyond this, treatment depends on the type and severity of the hemorrhoid, as well as how it has responded to any previous treatment. Hemorrhoids are divided into four grades (stages) depending on their history. Grade I and II hemorrhoids are usually treated nonsurgically, whereas Grades III and IV are more likely to be treated surgically.
01. Rubber Band Ligation (RBL)
Gastroenterology and Nutrition, P.C.
An elastic band is wrapped around the hemorrhoid, cutting off its blood supply, and causing the tissue to die and drop off. External hemorrhoid and early-stage internal hemorrhoids can be treated with RBL.
02. Infrared Photocoagulation (IPC) or Electrocoagulation
The hemorrhoid is exposed to a warm, painless infrared light or electrical current during a series of treatment sessions.
03. Injection Sclerotherapy
A sclerosing solution injected into the blood vessels causes the hemorrhoids to shrink.
04. Surgical Hemorrhoidectomy
Surgery is usually reserved for very advanced cases with a large amount of protrusion. The hemorrhoid is removed with a scalpel, cautery device or laser. Local or general anesthesia may be used, and hospitalization is usually required, with recovery taking up to 2 weeks.
05. Stapled Hemorrhoidectomy
This recently introduced procedure involves the insertion of a circular stapler into the rectum that pushes internal and external hemorrhoids and surrounding tissue up into the anal canal and staples them in place, cutting off blood supply.
More than half of adults in America have hemorrhoids. Few report them to their doctors, however, whether out of embarrassment or the belief that the only treatment is surgical removal. Patients should keep in mind that, the sooner hemorrhoids are diagnosed, the greater the chance that they can be treated with an in-office, nonsurgical procedure.
Hemorrhoid Treatment During Colonoscopy: A Two-in-One Approach
If you’re scheduling a colonoscopy and you also have hemorrhoid symptoms (rectal bleeding, itching, discomfort, or a noticeable lump), there’s a good chance we can treat both during the same visit. Combining your screening colonoscopy with hemorrhoid treatment saves you a separate appointment, a separate prep day, and a separate recovery period.
Which Hemorrhoids Can Be Treated During a Colonoscopy?
The procedures we perform during colonoscopy are designed for internal hemorrhoids, which are the type that form inside the rectum above the dentate line. Internal hemorrhoids are graded I through IV based on severity:
- Grade I (mild): May not need treatment beyond dietary changes, but rubber band ligation can be effective during colonoscopy if symptoms warrant
- Grade II (moderate): The most common candidate for rubber band ligation during colonoscopy
- Grade III (significant): Often treated with banding during colonoscopy, may need follow-up sessions
- Grade IV (severe): Usually requires a separate surgical referral, not a candidate for in-procedure treatment
Your gastroenterologist will assess your hemorrhoids during the colonoscopy and recommend the right treatment approach based on what we see.
External hemorrhoids (those that form below the dentate line, around the anus) generally cannot be treated during colonoscopy. They need a separate evaluation and may require different treatments such as topical medications, lifestyle changes, or in some cases surgical removal.
Treatment Methods Performed During Colonoscopy
The same in-office hemorrhoid treatments we offer can be performed while you’re already sedated and prepped for colonoscopy:
Rubber Band Ligation (RBL). A small rubber band is placed around the base of the internal hemorrhoid, cutting off its blood supply. The hemorrhoid shrinks and falls off within about a week. RBL is the most common method used during colonoscopy because it’s quick, effective, and doesn’t require additional anesthesia beyond the colonoscopy sedation you’re already receiving.
Infrared Coagulation (IRC). A short pulse of infrared light is directed at the hemorrhoid, creating scar tissue that cuts off the blood supply. IRC is particularly effective for smaller internal hemorrhoids and bleeding hemorrhoids. The procedure adds only a few minutes to your colonoscopy.
Sclerotherapy. A solution is injected into the hemorrhoid to shrink it. This is sometimes used for hemorrhoids that aren’t ideal candidates for banding.
The choice of method depends on the grade and location of your hemorrhoids. Your gastroenterologist makes the call based on what’s seen during the procedure.
Why Combine the Procedures
There are real practical reasons patients choose to combine:
- One prep day, not two. Colonoscopy prep is the hardest part of the procedure. Doing both in one visit means going through prep once.
- One sedation, not two. Sedation recovery is the same whether the procedure is 25 minutes or 30 minutes. You’re not signing up for additional sedation risk.
- One day off work. Most patients need a day off for colonoscopy. Combining means you don’t need a second day off later.
- One copay or deductible. Insurance billing for combined procedures is typically more efficient than separate appointments.
- Faster relief. If you’ve been putting off hemorrhoid symptoms because you didn’t want to schedule a separate appointment, combining means relief starts immediately after recovery.
Is This Right for Everyone?
Not always. Your gastroenterologist will discuss whether combining makes sense for you based on the grade and type of your hemorrhoids, your overall health and any conditions that affect sedation, whether you have other concerns (diverticulosis, polyps, IBD) that might affect the screening, and your preference.
If we determine that your hemorrhoid case needs surgical referral or a different treatment approach, we’ll tell you. The goal is the right treatment, not the most convenient one.
To combine procedures, mention your hemorrhoid symptoms when you call to schedule your colonoscopy. This lets our team plan for the additional time and confirm the treatment is appropriate before your visit. Call (718) 261-0900.
When to See a Doctor
Don’t ignore rectal bleeding. While hemorrhoids are the most common cause, bleeding can also point to anal fissures, polyps, or colorectal cancer. See a gastroenterologist if you experience:
- Rectal bleeding that lasts more than a few days
- Heavy bleeding or blood clots
- Changes in bowel habits along with bleeding
- A lump near the anus that grows or becomes increasingly painful
- Hemorrhoid symptoms that don’t improve with home treatment after two weeks
- Severe pain, especially sudden onset
If you’re over 45 and haven’t had a screening colonoscopy, rectal bleeding is a strong reason to schedule one. Our team at Gastroenterology and Nutrition, P.C. can evaluate your symptoms and rule out anything more serious. Call us at (718) 261-0900.
Common Questions About Hemorrhoids
Q: Can hemorrhoids cause stomach pain?
A: Hemorrhoids typically don’t cause stomach pain. They affect the rectum and anus, so symptoms stay in that area: rectal bleeding, itching, and localized discomfort. If you’re experiencing stomach or abdominal pain along with rectal symptoms, something else may be going on. Conditions like irritable bowel syndrome, inflammatory bowel disease, or infections can cause both. It’s worth getting evaluated to identify the real source.
Q: Can hemorrhoids be removed during a colonoscopy?
A: No. Hemorrhoids aren’t removed during a colonoscopy. A colonoscopy is a diagnostic procedure designed to examine the colon’s lining and remove polyps. Hemorrhoid treatment requires separate procedures like rubber band ligation or infrared coagulation. However, your gastroenterologist may notice hemorrhoids during a colonoscopy and recommend a treatment plan afterward. The two are often scheduled in coordination.
Q: How long does it take for hemorrhoids to go away?
A: Mild hemorrhoids often improve within a week or two with home care: more fiber, more water, sitz baths, and avoiding straining. Thrombosed external hemorrhoids typically take two to three weeks to resolve. After rubber band ligation, the treated hemorrhoid falls off within 5-7 days, with full healing in about two weeks. Chronic or recurring hemorrhoids may need ongoing management or a procedure.
Q: What is the best sleeping position for hemorrhoids?
A: Sleeping on your side is generally the most comfortable position when you have hemorrhoids. This reduces pressure on the rectal veins compared to sleeping on your back. Placing a pillow between your knees can help align your hips and reduce additional pressure. Avoid sleeping on your stomach, which can increase abdominal pressure. Elevating your legs slightly with a pillow can also improve blood flow and reduce swelling.
Q: Do hemorrhoids go away on their own?
A: Small, mild hemorrhoids can resolve on their own within a few days to a couple of weeks, especially with dietary changes and proper hygiene. However, larger hemorrhoids or those that prolapse often need treatment. Recurring hemorrhoids rarely go away permanently without some form of intervention. If your symptoms come back frequently, an in-office procedure like rubber band ligation can provide lasting relief.
Q: Can I get hemorrhoid treatment during my colonoscopy screening?
A: For most internal hemorrhoids, yes. We can perform rubber band ligation, infrared coagulation, or sclerotherapy during your colonoscopy without additional sedation or a separate appointment. External hemorrhoids and severe (Grade IV) internal hemorrhoids usually need a separate evaluation. Mention your hemorrhoid symptoms when you schedule so we can plan accordingly.
Q: Does insurance cover hemorrhoid treatment during a colonoscopy?
A: Most insurance plans cover both screening colonoscopy and medically necessary hemorrhoid treatment. Coverage details vary by plan and by whether the treatment is considered diagnostic or therapeutic. Our front desk verifies your specific benefits before your visit. Call (718) 261-0900 with your insurance information.
Q: Will my colonoscopy take longer if I'm getting hemorrhoid treatment too?
A: Slightly. A standard screening colonoscopy at our Forest Hills office typically takes 20 to 30 minutes. Adding rubber band ligation or infrared coagulation usually adds 5 to 15 minutes depending on how many hemorrhoids are treated. The recovery time is the same.
Q: How quickly will I feel relief from hemorrhoid treatment done during colonoscopy?
A: Most patients notice improvement within a week as the treated hemorrhoid shrinks and falls off. Banded hemorrhoids typically resolve in 7 to 10 days. You may have mild discomfort or a feeling of pressure in the first day or two after the procedure, which is normal.
Disclaimer: This information is provided for educational purposes and is not a substitute for professional medical advice, diagnosis, or treatment. Please schedule a consultation with our team to discuss your individual needs.
