Medically reviewed by Dr. Samuel Davidoff, MD, Board-Certified Gastroenterologist & Hepatologist | 18+ Years Experience | Last Updated: April 2026
Quick Answer
No, hemorrhoids do not cause bloating, gas, or pain in the lower abdomen. Hemorrhoids are inflamed blood vessels around the anus that cause pain locally, near the bottom, not higher up in the belly. If you have hemorrhoids and you also have abdominal bloating, gas, or lower-belly pain, those symptoms are coming from a separate issue (most commonly IBS, constipation, dietary triggers, food intolerance, or in rarer cases inflammatory bowel disease or colorectal pathology) that should be evaluated by a gastroenterologist. The two can occur together but are not causally linked.
Many patients with hemorrhoids also notice abdominal bloating, gas, or a heavy feeling in the lower abdomen and assume the two are connected. They almost never are. Hemorrhoids are a localized vascular problem at the anus. Bloating and lower abdominal symptoms come from the digestive tract higher up. Treating one will not resolve the other, and conflating them often leads to delayed diagnosis of the actual cause of the abdominal symptoms.
This guide explains why the two are anatomically and physiologically separate, what does cause those abdominal symptoms, when both can be present at the same time without being related, and when to come in for evaluation.
The Direct Answer From Our Gastroenterologist
Per Dr. Yuriy Israel, MD, board-certified gastroenterologist at Gastroenterology and Nutrition P.C.:
“No, hemorrhoids cause pain locally around your anus. If you’re experiencing stomach pain, it is likely due to another issue that needs to be addressed.”
Dr. Yuriy Israel, MD, Board-Certified Gastroenterologist, Forest Hills
That single answer applies equally to bloating, gas, lower abdominal pain, and any other symptom located above the anal canal.
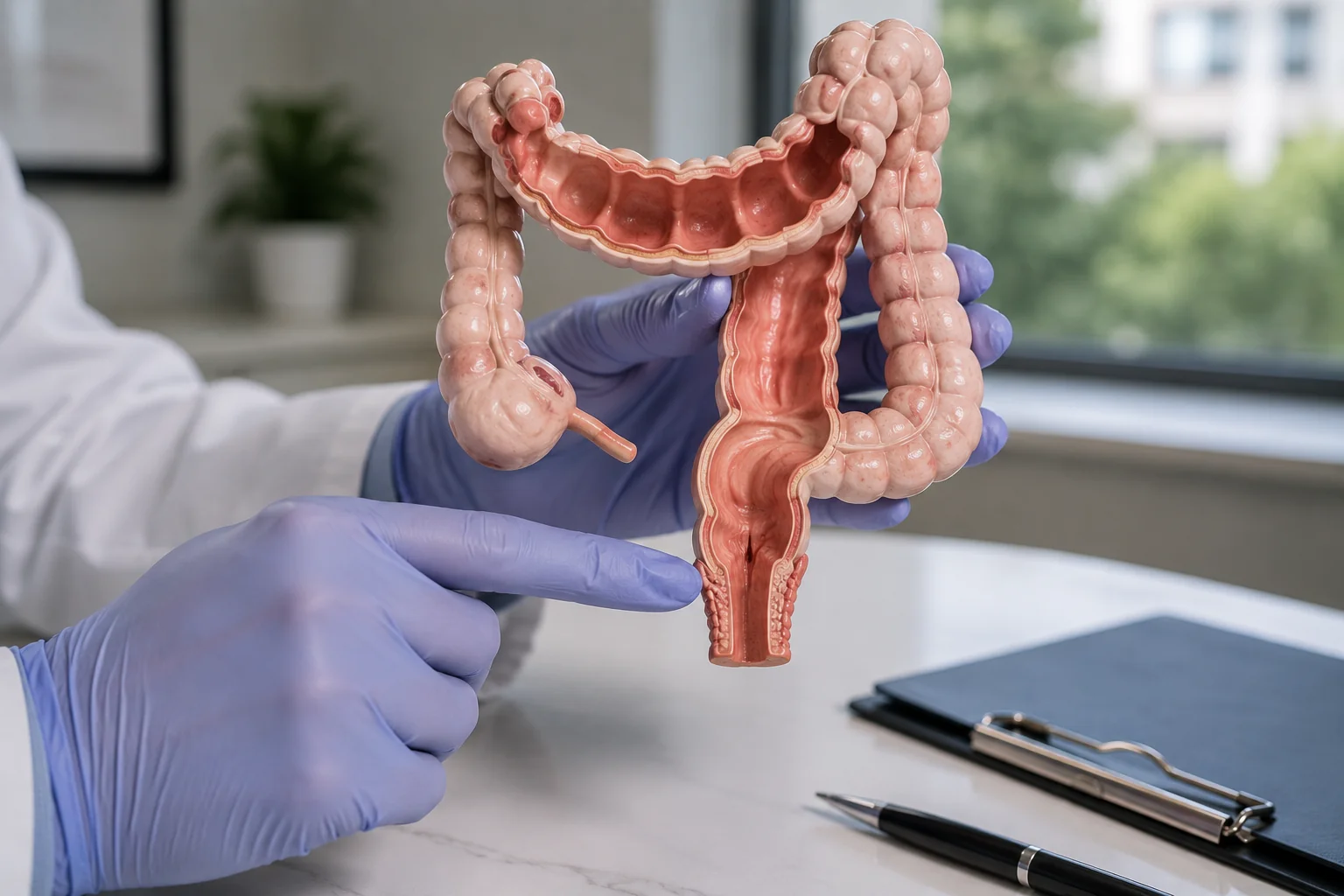
What Hemorrhoids Actually Are (and Where the Pain Comes From)
Hemorrhoids are clusters of blood vessels in the wall of the rectum and anus. Everyone has them. They become a clinical problem only when they become inflamed, swollen, or thrombosed (a blood clot forms inside one). The two main types:
- Internal hemorrhoids sit inside the rectum, above a region called the dentate line. They generally do not cause pain because the area lacks pain-sensing nerve fibers. They can bleed (bright red blood on toilet paper or in the bowl after a bowel movement) and can prolapse (drop down into the anal canal).
- External hemorrhoids sit just outside the anus, below the dentate line, in skin that is rich in pain nerves. When they swell or thrombose, they cause sharp, localized anal pain that is worse with sitting, walking, and bowel movements.
Per Dr. Israel: “Hemorrhoids cannot cause cancer. They are blood vessels that get inflamed and cause local pain around the anus.”
The key word is local. The vascular and nerve anatomy of hemorrhoids stops at the anus. There is no anatomical pathway by which a swollen anal blood vessel can cause gas in the small intestine, bloating in the colon, or cramping in the lower abdomen.
What Actually Causes Abdominal Bloating, Gas, and Lower Belly Pain
If you have hemorrhoids and you also have abdominal symptoms, the abdominal symptoms have a different cause. The most common culprits in our Forest Hills practice:
Irritable bowel syndrome (IBS)
The most common cause of bloating + gas + lower abdominal pain in adults. IBS is a functional disorder of the gut where the bowel is hypersensitive and motility is irregular. Symptoms vary by subtype (IBS-C with constipation, IBS-D with diarrhea, IBS-M mixed). The treatment is dietary modification, fiber adjustment, sometimes medications targeting motility or visceral pain.
Constipation
Slow stool transit causes gas to build up, the abdomen to distend, and the lower belly to feel heavy. Chronic constipation is also one of the leading causes of hemorrhoids (straining at stool engorges the anal vessels), which is why the two often appear together. Fixing the constipation usually fixes both.
Food intolerance (lactose, fructose, FODMAPs)
Undigested sugars in the small intestine ferment in the colon, producing gas, bloating, and cramping. Lactose intolerance is the most common; FODMAP intolerance is increasingly recognized.
Small intestinal bacterial overgrowth (SIBO)
An imbalance of bacteria in the small intestine that produces excess gas during digestion. Diagnosed with a breath test. Treated with targeted antibiotics.
Inflammatory bowel disease (Crohn’s disease and ulcerative colitis)
Chronic inflammation of the digestive tract that can cause abdominal pain, bloating, diarrhea, and weight loss. Different from hemorrhoids, but Crohn’s disease can affect the perianal area and produce features that resemble hemorrhoids (perianal abscesses, fistulas, skin tags). If you have abdominal symptoms plus complex perianal disease, an IBD evaluation is warranted.
Celiac disease
An autoimmune reaction to gluten that damages the small intestine and causes bloating, abdominal pain, diarrhea, and nutrient deficiencies. Diagnosed with blood work and confirmed with biopsies during upper endoscopy.
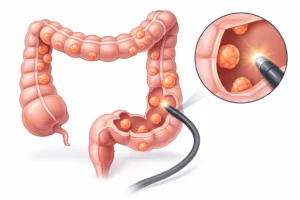
Colorectal pathology
Polyps and colorectal cancers can produce abdominal pain, blood in the stool, and changes in bowel habits that are sometimes attributed to hemorrhoids. This is why it is important not to assume bleeding is “just hemorrhoids” without an evaluation, especially if you are over 45 or have risk factors for colon cancer.
When Both Can Be Present (Without Being Related)
It is very common for a single patient to have both hemorrhoids and abdominal symptoms. Here is why the two often coexist without one causing the other:
- Constipation drives both. Slow transit causes bloating and gas in the abdomen, and the straining causes hemorrhoids at the anus.
- Pregnancy drives both. Hormonal changes slow digestion (bloating + constipation), and the growing uterus increases pelvic venous pressure (hemorrhoids).
- Sedentary lifestyle drives both. Reduced gut motility leads to bloating and gas, and prolonged sitting aggravates hemorrhoids.
- Low-fiber diet drives both. Hard stools cause straining (hemorrhoids) and slow transit (bloating, gas).
The fact that they share underlying drivers explains why the two often appear at the same time but are not causally linked.
Symptoms That Are Truly Hemorrhoid-Related
To distinguish hemorrhoid symptoms from abdominal symptoms, here is the actual hemorrhoid symptom profile:
- Bright red blood on toilet paper or in the bowl after a bowel movement (internal hemorrhoid bleeding)
- Pain or itching at the anus, especially after sitting or bowel movements (external)
- A tender lump or swelling at the anus (thrombosed external hemorrhoid)
- A sense of fullness or pressure at the anus, sometimes with a soft tissue protrusion that retracts on its own (internal hemorrhoid prolapse)
- Mild mucus or staining at the anus
- Discomfort that is worse with sitting on hard surfaces, prolonged toilet sitting, or straining
Symptoms that are NOT hemorrhoid-related (need separate evaluation):
- Bloating
- Gas
- Lower abdominal pain or cramping
- Upper abdominal pain or heartburn
- Nausea or vomiting
- Diarrhea or chronic constipation
- Unintentional weight loss
- Fever
- Pencil-thin stools or other major bowel habit changes
When to Come In for Evaluation
Schedule a gastroenterology consultation if you are experiencing any of the following:
- Abdominal bloating, gas, or pain that is persistent or recurrent
- Rectal bleeding that you have been “blaming on hemorrhoids” but have not had evaluated, especially if you are 45 or older
- Bowel habit changes (new constipation, new diarrhea, alternating, or pencil-thin stools)
- Unintentional weight loss
- Symptoms that disrupt sleep, work, or social activities
- Hemorrhoid symptoms that are not improving with conservative measures (fiber, hydration, sitz baths, OTC creams) within 3 to 4 weeks
Per Dr. Davidoff: “Rectal bleeding, unintentional weight loss, new-onset unprovoked constipation or diarrhea, or any change in bowel habit” are red flags that warrant an evaluation, not symptoms to wait out.
What an Evaluation Typically Involves
For a patient with both hemorrhoid symptoms and abdominal symptoms, the typical workup at our Forest Hills practice:
- Detailed history and physical exam, including an anal exam to characterize the hemorrhoids.
- Blood work to look for anemia (suggests blood loss), inflammatory markers (suggests IBD), celiac antibodies if indicated.
- Stool tests for bacterial pathogens, parasites, calprotectin (marker of intestinal inflammation), or fecal occult blood.
- Colonoscopy if you are over 45, have rectal bleeding, or have any of the red-flag symptoms above. The colonoscopy directly visualizes the entire colon and treats both diagnostic and screening goals at the same time.
- Upper endoscopy if upper abdominal symptoms (heartburn, upper abdominal pain, suspected celiac, suspected H. pylori) are present.
- Targeted treatment for both the hemorrhoids and the underlying GI issue once the diagnosis is clear.
Per Dr. Davidoff on our diagnostic approach: “We tailor our approach to each and every patient. We start with obtaining a thorough history and doing a targeted physical exam. Depending on the patient’s symptoms and history, we then can proceed with blood work, stool tests, imaging studies as well as endoscopic evaluation; all depending on what exactly is going on with that specific patient.”
Hemorrhoid Treatment While the Abdominal Workup Is Underway
The two issues can be treated in parallel. Conservative hemorrhoid management can begin immediately while the abdominal evaluation is in progress:
- High-fiber diet (25 to 35 grams per day from food and supplements)
- Adequate hydration (typically 64 to 80 ounces of water per day)
- Avoid straining or prolonged sitting on the toilet
- Sitz baths (warm water soak of the anal area for 10 to 15 minutes, several times per day)
- OTC topical hydrocortisone or witch hazel pads for symptomatic relief
- OTC numbing creams (lidocaine) for pain
- Stool softeners if constipation is a driver
Per Dr. Israel: “External hemorrhoids usually take about three to four weeks to fully go away, provided you avoid aggravating them. Pushing and straining due to constipation, heavy lifting, or prolonged sitting can aggravate hemorrhoids. Maintaining soft stools with laxatives and avoiding heavy lifting can help them heal faster.”
Why Forest Hills Patients Choose Our Practice
Gastroenterology and Nutrition P.C. is an AAAASF-certified facility at 108-16 72nd Avenue, 2nd Floor, Forest Hills, Queens NY 11375. Our team handles the full range of gastrointestinal issues including hemorrhoids, IBS, IBD, colorectal cancer screening, and on-site upper endoscopy and colonoscopy. We offer Sunday hours for patients who need weekend appointments and accept most commercial insurances, Medicare, and various Medicaids. Our team speaks English, Russian, and Spanish.
If you have been attributing abdominal symptoms to hemorrhoids, or if you have hemorrhoid symptoms that are not improving, schedule a consultation. Same-week appointments are usually available.
Schedule a Gastroenterology Consultation
Or call (718) 261-0900
Frequently Asked Questions
Can hemorrhoids cause gas?
No. Hemorrhoids are localized blood vessels at the anus and have no role in digestion or gas production. If you are experiencing gas, the cause is in the digestive tract upstream from the anus and should be evaluated separately.
Can hemorrhoids cause lower abdominal pain?
Per Dr. Israel: “No, hemorrhoids cause pain locally around your anus. If you’re experiencing stomach pain, it is likely due to another issue that needs to be addressed.” Lower abdominal pain has many possible causes (IBS, constipation, IBD, urinary or gynecologic issues) and warrants its own evaluation.
Can hemorrhoids cause bloating?
No. Bloating is a sign of intestinal gas distention, slow transit, food intolerance, or other GI disorder. It is not produced by anal vascular swelling.
Can hemorrhoids cause cancer?
Per Dr. Israel: “Hemorrhoids cannot cause cancer. They are blood vessels that get inflamed and cause local pain around the anus.” However, rectal bleeding should never be attributed to hemorrhoids without evaluation, because colorectal cancers can also bleed and the symptoms can look identical from the patient’s perspective.
I have both hemorrhoids and bloating. Is that unusual?
Not at all. Both share underlying causes like constipation, low-fiber diet, sedentary lifestyle, and pregnancy. The two often appear together but are not causally linked. Treating the underlying driver (e.g., the constipation) often improves both at the same time.
How long do hemorrhoids take to go away?
Per Dr. Israel: “External hemorrhoids usually take about three to four weeks to fully go away, provided you avoid aggravating them.” Persistent or recurrent hemorrhoids may need in-office treatment (banding, injection therapy) or, in select cases, surgical removal.
This information is provided for educational purposes and is not a substitute for professional medical advice, diagnosis, or treatment. Please schedule a consultation with our team to discuss your individual needs.