Medically reviewed by Dr. Samuel Davidoff, MD – Board-Certified Gastroenterologist & Hepatologist | 15+ Years Experience | Last Updated: April 2026
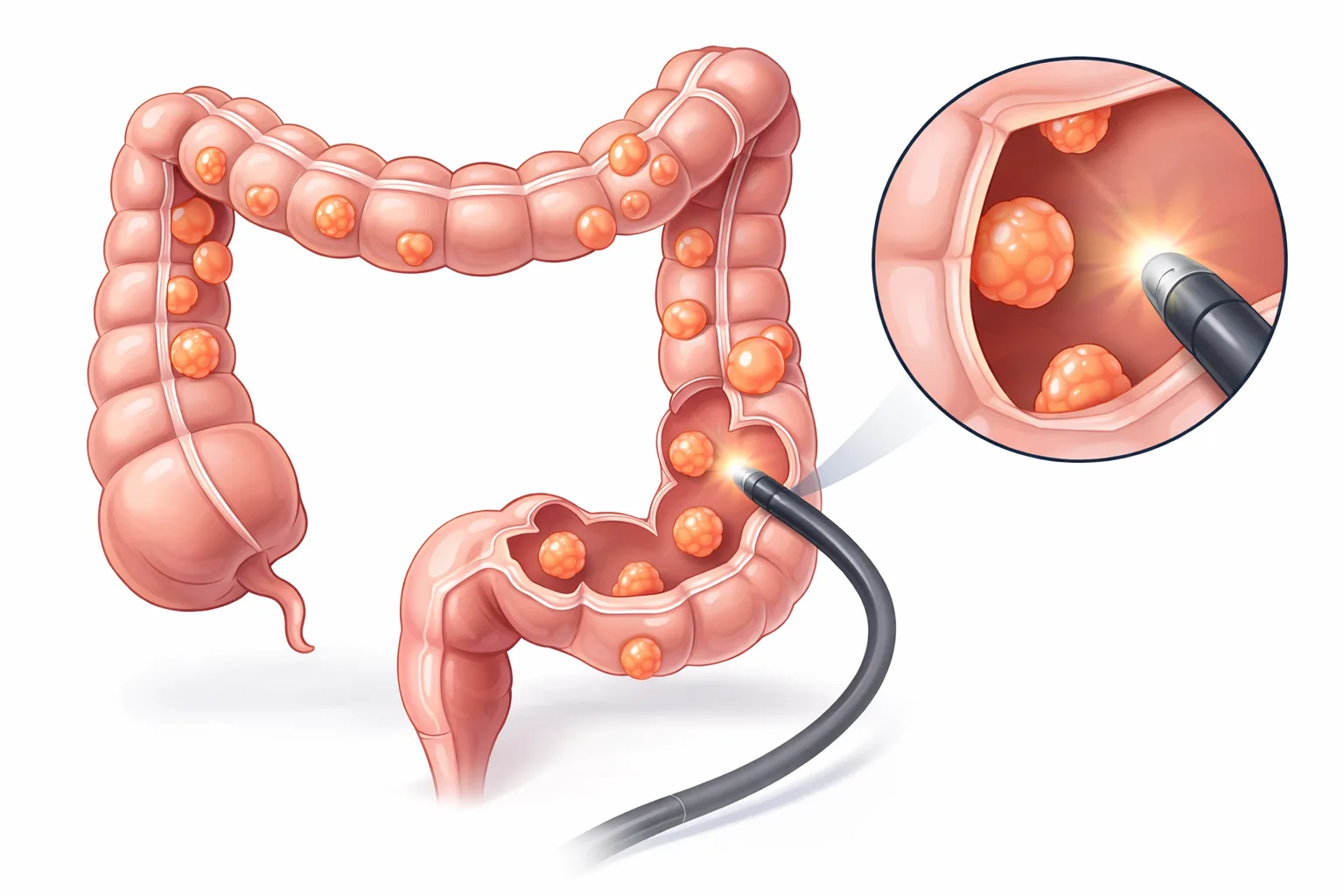
Colon polyps form when cells in the lining of the colon grow abnormally and do not follow the normal process of cell replacement. Instead of old cells dying and being replaced in an orderly way, extra cells accumulate and form growths on the colon wall. While the exact cause of this abnormal cell growth is not fully understood, several factors increase the risk, including age, family history, lifestyle choices like smoking and diet, and certain inherited genetic conditions.
Most colon polyps are harmless, but some types can develop into colorectal cancer over time. This is why understanding what causes polyps and knowing your risk factors is so important. Regular colonoscopy screenings allow doctors to find and remove polyps before they become cancerous, making prevention possible.
How Colon Polyps Develop
The colon is lined with millions of cells that regularly die and are replaced with new ones. This process is tightly controlled by genes that tell cells when to grow, divide, and die. When something disrupts this process, cells may continue to grow when they should stop, forming a small clump of tissue called a polyp.
Polyps can develop anywhere in the large intestine, including the colon and rectum. They vary in size, shape, and type. Some polyps are flat, while others are raised on a stalk. Most polyps grow slowly over many years, which is why regular screening can catch them early.
The transformation from a normal cell to a polyp to cancer typically takes 10 to 15 years. This slow progression gives doctors a significant window of opportunity to detect and remove polyps before they become dangerous.
Risk Factors That Increase Your Chances of Developing Colon Polyps
While anyone can develop colon polyps, certain factors increase the likelihood. Understanding these risk factors can help you take steps to reduce your risk and ensure you get screened at the right time.
Age
The risk of colon polyps increases significantly after age 45. Most people who develop polyps are 50 or older. As the body ages, cells are more likely to develop mutations that lead to abnormal growth. This is why screening guidelines recommend beginning colonoscopies at age 45 for people at average risk.
Family History
If a parent, sibling, or child has had colon polyps or colorectal cancer, your risk is higher. The risk increases further if multiple family members have been affected or if they were diagnosed at a young age.
“Patients who have a first or second degree relative with colon cancer should start doing screening colonoscopies at age 40 or 10 years prior to the age that relative was diagnosed, whichever comes first.”
– Dr. Samuel Davidoff, MD, Board-Certified Gastroenterologist
Personal History of Polyps
If you have had colon polyps before, you are more likely to develop new ones. This is why follow-up colonoscopies are scheduled at regular intervals after polyps are found and removed.
Inflammatory Bowel Disease
Having ulcerative colitis or Crohn’s disease increases the risk of colon polyps and colorectal cancer. Long-term inflammation in the colon can lead to changes in the cells that line the intestine. People with IBD typically need more frequent colonoscopies.
Obesity
Being significantly overweight increases the risk of both developing colon polyps and dying from colorectal cancer. Excess body fat, particularly around the waist, is associated with higher levels of insulin and other hormones that may promote abnormal cell growth.
Smoking
Smokers have a significantly higher risk of developing colon polyps compared to nonsmokers. The chemicals in tobacco smoke can cause DNA damage in cells throughout the body, including the colon. Learn more about the link between smoking and colorectal cancer.
Alcohol Consumption
Drinking three or more alcoholic beverages per day increases the risk of colon polyps. The combination of alcohol and smoking raises the risk even further.
Diet
A diet high in red and processed meats and low in fiber, fruits, and vegetables is associated with increased polyp risk. Fiber helps move waste through the colon more quickly, reducing the time that potentially harmful substances are in contact with the colon lining.
Other Risk Factors
Lack of physical activity, type 2 diabetes, and certain racial factors also increase risk. In the United States, Black Americans have a higher risk of developing colorectal cancer and may benefit from earlier and more frequent screening.
Types of Colon Polyps and Which Ones Can Become Cancer
Not all colon polyps are the same. Understanding the different types can help you understand your risk if polyps are found during a colonoscopy.
| Polyp Type | Cancer Risk | Notes |
|---|---|---|
| Tubular adenomas | Lower risk | Most common precancerous polyp type |
| Villous adenomas | Higher risk | Less common, especially dangerous when large |
| Sessile serrated lesions | Moderate risk | Flat, hard to detect, often in right colon |
| Hyperplastic polyps | Very low | Common, almost never cancerous |
| Inflammatory polyps | Not directly | Occur in IBD patients, indicate chronic inflammation |
When polyps are removed during a colonoscopy, they are sent to a laboratory for analysis. The pathology report identifies the type and whether any concerning changes are present. This information helps your gastroenterologist determine how often you need follow-up colonoscopies.
Can You Prevent Colon Polyps?
While you cannot control all risk factors like age and family history, several lifestyle changes can help reduce your risk:
- Eat a high-fiber diet with plenty of fruits, vegetables, whole grains, and legumes
- Limit red and processed meats – consider replacing some with fish, poultry, or plant-based proteins
- Maintain a healthy weight – even modest weight loss helps reduce risk
- Exercise regularly – aim for at least 30 minutes of moderate activity most days
- Limit alcohol to one drink per day for women and two for men
- Do not smoke – quitting is one of the best things you can do for your colon health
- Get screened on time – the most effective way to prevent colorectal cancer
How Colon Polyps Are Found and Removed
Colonoscopy is the gold standard for detecting and removing colon polyps. During a colonoscopy, a gastroenterologist uses a flexible tube with a camera to examine the entire colon. If polyps are found, they can be removed during the same procedure.
“A screening colonoscopy is the mainstay for prevention of colon cancer. If a patient undergoes a screening colonoscopy on time and a polyp is found, it can be quickly removed, thereby preventing colon cancer.”
– Dr. Samuel Davidoff, MD
Most patients do not feel polyps being removed because the colon lining does not have pain nerves. The procedure is performed under sedation, so you are comfortable throughout.
How Often Should You Get a Colonoscopy If You Have Polyps?
If polyps are found during your colonoscopy, your gastroenterologist will recommend a surveillance schedule based on the number, size, and type of polyps removed:
- One or two small tubular adenomas: follow-up in 7 to 10 years
- Three or more adenomas, larger adenomas (10 mm+), or villous features: follow-up in 3 years
- Advanced findings or certain serrated polyps: more frequent surveillance
“In any condition, including gastrointestinal conditions, early detection is key and can help avoid bad outcomes and invasive or painful procedures.”
– Dr. Samuel Davidoff, MD
Colonoscopy and Polyp Removal at Gastroenterology and Nutrition, P.C.
At Gastroenterology and Nutrition, P.C. in Forest Hills, Queens, Dr. Samuel Davidoff, MD, and Dr. Yuriy Israel, MD, have performed over 10,000 colonoscopies. Both physicians are board-certified gastroenterologists with extensive experience in polyp detection and removal using high-definition colonoscopy technology.
“We then bring the patient into the procedure room, where they lay down on the bed and the anesthesiologist inserts an IV that will be used to put them to sleep,” explains Dr. Davidoff. “The procedure itself takes an average of about 15 to 20 minutes. When we reach the end of the colon, we start to slowly withdraw the colonoscope looking for polyps. If we find a polyp, we remove it right there and then.”
The office is located at 108-16 72nd Ave in Forest Hills, with appointments available Monday through Friday and Sunday mornings. The practice accepts most major insurance plans, including Medicare. Learn more about what causes colorectal cancer and how colorectal cancer is diagnosed.
To schedule a colonoscopy or consultation, call 718-261-0900.
Frequently Asked Questions
Are colon polyps common?
Yes, colon polyps are very common, especially in adults over 50. It is estimated that about 25% to 30% of adults will have at least one polyp found during a screening colonoscopy. The good news is that most polyps can be easily removed before they cause problems.
Do colon polyps cause symptoms?
Most colon polyps do not cause any symptoms, which is why screening is so important. In some cases, larger polyps may cause rectal bleeding, changes in bowel habits, or abdominal pain. Regular colonoscopy is the best way to find them.
At what age should I start screening for colon polyps?
For people at average risk, screening should begin at age 45. If you have a family history of colon polyps or colorectal cancer, or other risk factors, your doctor may recommend starting earlier. Talk to your gastroenterologist about when you should begin screening.
Can colon polyps grow back after removal?
Once a polyp is removed, that specific polyp will not grow back. However, new polyps can develop in other areas of the colon over time. This is why follow-up colonoscopies are recommended at regular intervals after polyps are found.
How can I reduce my risk of colon polyps?
You can reduce your risk by maintaining a healthy weight, eating a diet rich in fiber and low in red meat, exercising regularly, limiting alcohol, not smoking, and getting screened on time. While you cannot control factors like age and family history, these lifestyle changes can make a meaningful difference.
Medical Disclaimer: This article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult with a qualified healthcare provider regarding any medical concerns.